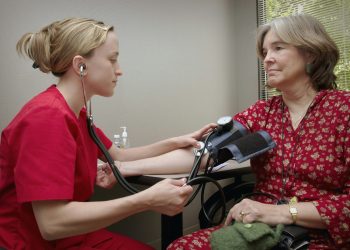
Shoulder mobility is vital to standard function of the body. The shoulder joint is complex, and it requires stability and control to move and perform properly. Often, patients experience instability and too much mobility in the shoulder. When this happens, the limb may move out of the joint or sit less tightly than it should, a condition known as shoulder instability.
What is Shoulder Instability?
For the shoulder to function properly, the ball of the shoulder must remain completely within the socket joint. When the ball pops out of the joint, even partially, the result may include limited mobility and function as well as serious pain. Shoulder subluxation occurs when the ball is partially out of the socket, and shoulder dislocation occurs when the ball is completely out of the socket.
The underlying cause of shoulder instability will often dictate which treatment is best in restoring functionality and eliminating pain.
Traumatic Injury
If a traumatic injury occurs, the ball and socket joint can become seriously compromised. This often occurs due to sports injury, fall, or other traumatic event. In this scenario, the shoulder must often be repositioned using specific movements designed to insert the ball into the socket with as little harm to the joint and surrounding areas as possible.
Multi-Directional Instability (MDI)
Multi-directional instability—or MDI—is a gradual degradation of the ball and socket joint. There is no traumatic event that triggers the instability, but it generally worsens over time. MDI might be the result of distinctive bone anatomy, such as having a shoulder socket that is naturally shallow or uniquely shaped. It could also result from a torn ligament or injured muscles around the shoulder. An untreated shoulder injury may, over time, result in MDI.
Symptoms of Shoulder Instability
Shoulder instability can be unnoticeable or extremely obvious. Patients may experience symptoms for a long period of time before recognizing there is an underlying issue. It is important to identify shoulder concerns early on to avoid permanent damage to the shoulder. Common symptoms of shoulder instability include:
- Pain
- Noticeable instability with shoulder-related activities
- Weakness in the shoulder
- Popping or grinding (feelings or sounds) in the shoulder
- The sensation of the shoulder “slipping” when used
Overhead movements may be especially challenging if you are experiencing shoulder instability.
Young athletes are particularly prone to shoulder instability, notably those who pitch in baseball or softball, play volleyball, or swim. Tennis players are also more susceptible to shoulder instability than those who play other sports. After one dislocation, chronic problems may result.
Improving Shoulder Instability
There are a number of procedures that may improve shoulder instability. The most conservative treatments implement anti-inflammatory medications and cortisone injections. Rehabilitation exercises can also be extremely useful in addressing range of motion limitations, building strength, and increasing shoulder control.
Minimally invasive surgical treatments are available when conservative treatment is ineffective. The nature of injury often dictates the preferred repair method.
Stopping at conservative treatment is never a good solution without consultation with your doctor. Treatment is often progressive, and stopping or delaying drug therapies, physical rehabilitation or surgery could result in further damage to the shoulder. The following are common repair methods for shoulder instability:
Bankart Repair
A Bankart repair addresses specific problems with the ligaments surrounding the shoulder joint. It consists of sewing or stapling the ligaments on the front side of the shoulder joint to restore their position prior to injury or gradual decline.
This repair can often be performed with just a small incision, making the recovery time faster and safer than more invasive procedures.
Capsular Shift
A capsular shift addresses loosening of the joint capsule. The shoulder capsule is a group of ligaments around the shoulder that stabilize it. When the envelope around the shoulder is loose, it increases the size of the shoulder capsule, allowing it to move more than it should. A capsular shift tightens the capsule around the shoulder.
This procedure is done in one of two ways:
- Through traditional surgery, which requires an incision in the front of the shoulder.
- Through arthroscopic surgery, which requires smaller incisions and the use of the camera.
In general, these smaller incisions will often decrease total recovery time.
Latarjet
The Latarjet procedure alters the shoulder dramatically. It is reserved for those who experience recurring instability. This procedure involves moving a small structure on the shoulder blade, the coracoid, to the front of the glenoid. It replaces missing bone and acts as a strut. Ultimately, the goal is to prevent further dislocations from occurring.
Once a common procedure to address shoulder dislocation, it has been replaced by other arthroscopic surgeries in all but the most severe instances of injury. Latarjet is a more invasive procedure used when the patient has worn away at least 25% of the shoulder socket. The recovery time increases to at least six weeks followed by extensive rehab.
Finding the Right Treatment for You
Determining the optimal treatment method for your injury and health goals falls to your physician. When devising a treatment plan, the orthopedic specialist considers your medical history, degree of instability, and underlying cause of injury to determine your treatment plan.
Prominent orthopedic surgeon, Dr. Brian Cable notes, “Shoulder injury is a pervasive concern in aging populations, athletes and those whose professions require repetitive upper extremity action. Early intervention and treatment can restore mobility and prevent permanent damage to the shoulder. The patient’s quality of life is of utmost priority, and a solid treatment plan is most effective when coupled with early detection.
Reach out to your physician with any concerns regarding shoulder pain and loss of mobility.